Translate this page into:
A case of toxin-induced neuromyotonia

*Corresponding author: Praveen Kumar Yadav, Department of Neurology, Aarogyam Neuroclinic, Durgapur, West Bengal, India. dr.praveen4u@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Yadav PK, Panda AK. A case of toxin-induced neuromyotonia. Med India 2023;2:18. doi: 10.25259/MEDINDIA_20_2023
Abstract
Neuromyotonia is a rare acquired neuromuscular disorder with autoantibodies manifesting as a paraneoplastic syndrome after certain neoplasms or after some toxin exposure. Toxins include heavy metal poisoning like mercury ingestion in the form of indigenous medicines. Here, we report a case of neuromyotonia in a patient pre-exposed to “Siddha” medicine.
Keywords
Neuromyotonia
Anti-voltage gated potassium channel antibody
Mercury
Siddha
Electromyography
INTRODUCTION
Neuromyotonia, or Isaac’s syndrome, is a rare neuromuscular disorder characterized by rippling muscle movements (myokymia), focal muscle hypertrophy, muscle stiffness, delayed muscle relaxation (pseudomyotonia), with electromyographic evidence of myokymic or neuromyotonic discharge,[1] Neuromyotonia is a form of acquired peripheral nerve hyperexcitability syndrome that is associated with neoplasms such as thymoma or mediated by toxins like heavy metal poisoning. Most cases show evidence of an autoimmune process in the form of an anti-voltage-gated potassium channel (VGKC) antibody.
CASE REPORT
A 35-year-old man with a skin lesion over his right lower limb presented with twitching of the right thigh muscle with frequent cramps and pain. After a detailed history, it was found that the patient was taking some “Siddha” medications (a type of traditional Indian medicine) for the skin lesion. Thigh pain and muscle cramps started after 1 month of ingestion of a prescribed dose of Ayurvedic medicine. The skin lesion was diagnosed as localized morphea by a dermatologist.
On examination, there was an involuntary movement of the right thigh and a bag of worm appearance. Figures 1 and 2 shows the skin lesions and the involuntary movements of the thigh. The patient had no sensory symptoms and no bladder involvement. Hence, the possibility of neuromyotonia was considered. The patient was followed up with needle electromyography (EMG). EMG showed waning neuromyotonic discharge. Due to the decrementing response in EMG of the right quadriceps muscle, the diagnosis of neuromyotonia was considered. Other causes of muscle fasciculation and peripheral nerve hyperexcitability were evaluated. Serum creatine phosphokinase (CPK), inflammatory markers, thyroid hormone profile, and blood sugar were done. Laboratory reports revealed normal levels of CPK, erythrocyte sedimentation rate, and C-reactive protein.

- Skin lesions diagnosed as morphea.
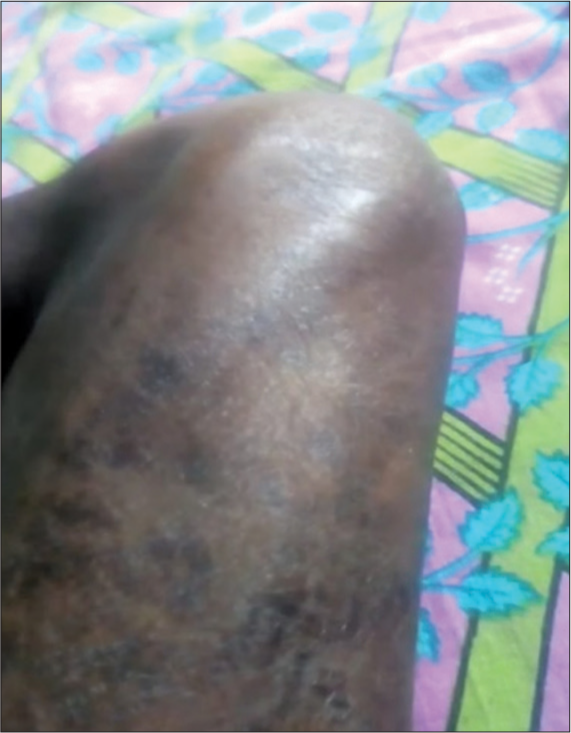
- Twitching of thigh muscles.
Further evaluation with specific antibodies such as an anti-VGKC antibody, anti-contactin associated protein like (CASPR) ab, and anti-leucine-rich glioma inactivated protein 1 (LGI1) antibody was done. The VGKC antibody came positive. Computed tomography chest and abdomen and ultrasonography of the thyroid and scrotum were done to rule out paraneoplastic causes. The possibility of toxic neuromyotonia was surveyed. Composition analysis of Ayurvedic medicine showed high mercury content. Therefore, a diagnosis of mercury-induced toxic neuromyotonia was established. The culprit agent was then discontinued and the patient’s movements were improved.
DISCUSSION
Neuromyotonia is a type of peripheral nerve hyperexcitability syndrome that was first described by Hyam Isaacs; hence known as Isaacs’s syndrome. The term “Neuromyotonia” was first used by Mertens and Zschocke in 1965 and subsequently “neuromyotonia” is being used as a generic term for peripheral nerve excitability syndrome.[2] Patients with neuromyotonia show symptoms like muscle twitching at rest, that is, myokymia and muscle cramps, which get triggered by voluntary or induced muscle contractions along with impaired muscle relaxation that persists even during sleep.[1,3,4] EMG recording shows short semirhythmic bursts of spontaneous, continuous, and irregularly happening doublet, triplet, or multiplet single motor unit discharges, firing at neuromyotonic ange (150–250 Hz), or myokymic range (5–60 Hz) followed by a few seconds of silence with pinging sound on loudspeaker. Other findings include fibrillation potentials and fasciculations.[4-6]
Often neuromyotonia is considered a paraneoplastic syndrome because it is associated with neoplasms such as thymoma and small-cell lung cancer.[5,7] This disorder is sometimes referred to as acquired neuromyotonia or idiopathic generalized myokymia. Most of the patients with Isaacs syndrome are anti-VGKC antibody positive; hence, respond to immunomodulation therapy such as plasmapheresis, steroid, and azathioprine. Anti-VGKC antibodies are actually directed at proteins surrounding the potassium channel rather than the channel itself; thus, they are now known as VGKC complex antibodies.[5,7] These cell-surface autoantibodies are directed against LGI1 and CASPR2. Differential diagnosis of VGKC complex antibody-positive peripheral nerve hyperexcitability syndrome includes Cramp-Fasciculation syndrome, Morvan syndrome, and Limbic encephalitis.[7] Morvan syndrome also known as maladie de Morvan presents with peripheral nerve excitability and autonomic instability, similar to Isaacs syndrome but symptoms of encephalopathy differentiate this from neuromyotonia.[8]
Several cases of neuromyotonia syndrome associated with exposure to toxic metals such as gold, mercury, lithium, and platinum have been studied.[6,9,10] A case report in India showed that an anti-CASPR2 antibody was detected in 12 out of 32 patients of clinical neuromyotonia due to chronic mercury toxicity following intake of unauthorized Siddha medicine.[11] Treatment options include low-to-moderate dosing of carbamazepine or phenytoin. Unresponding and antibody-positive cases with severe symptoms require IV immunoglobulin and plasmapheresis.
CONCLUSION
This case may suggest the significance of autoimmune antibodies (anti-LGI1 and anti-CASPR2 antibodies) in the pathogenesis of neuromyotonia syndrome due to the intake of mercury in the form of indigenous medication. Mercury could work as a trigger factor of the autoimmune antibodies, thereby leading to peripheral nerve excitability. Further studies are required to clarify the mechanism of activation of autoimmune antibodies. In recent onset neuromyotonia in adults, proper drug history should be taken especially indigenous or complementary systems of medicines and other toxic substances.
Author contributions
Praveen Kumar Yadav:Patient data collection, writing the manuscript. Ashwini Kumar Panda: Patient data collection, writing the manuscript.
Declaration of patient consent
Patient’s consent was not required as the patients identity was not disclosed or compromised.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Nil.
References
- A syndrome of continuous muscle-fibre activity. J Neurol Neurosurg Psychiatry. 1961;24:319-25.
- [CrossRef] [PubMed] [Google Scholar]
- Neuromyotonia as an unusual neurological complication of primary Sjögren's syndrome: Case report and literature review. Clin Rheumatol. 2017;36:481-4.
- [CrossRef] [PubMed] [Google Scholar]
- Immune-associated neuromyotonia syndrome following mercury poisoning. Neurol Sci. 2021;42:1583-6.
- [CrossRef] [PubMed] [Google Scholar]
- Peripheral nerve hyperexcitability syndromes. Continuum (Minneap Minn). 2017;23:1437-50.
- [CrossRef] [PubMed] [Google Scholar]
- De la choree fibrillaire per de Dr Morvande Lannills. Gaz Hebd Med Chir. 1890;15:173-6.
- [Google Scholar]
- Rheumatoid rigor: Gold induced myokymia. A report and review of the literature. J Rheumatol. 1986;13:195-6.
- [Google Scholar]
- Detecting acute neurotoxicity during platinum chemotherapy by neurophysiological assessment of motor nerve hyperexcitability. BMC Cancer. 2010;10:451.
- [CrossRef] [PubMed] [Google Scholar]
- Mercury toxicity following unauthorized siddha medicine intake-a mimicker of acquired neuromyotonia-report of 32 cases. Ann Indian Acad Neurol. 2018;21:49-56.
- [CrossRef] [PubMed] [Google Scholar]






